Breastfeeding Potentially Lowers Maternal Risk of Cardiovascular Events

Introduction:
Studies have shown that aside from its health effects on babies, breastfeeding also positively impacts maternal health. Breastfeeding has been strongly associated with decreased maternal risk of type 2 diabetes, breast and ovarian cancers.1 Meanwhile, the definite link between breastfeeding and cardiovascular diseases (CVD) has not been fully established. This systematic review and meta-analysis aim to address this gap, as it presents the association between breastfeeding and maternal risk for CVD events, including coronary heart disease (CHD), stroke, and fatal CVD.2
Methodology:
The systematic review included studies that assessed the association between breastfeeding history and incidence of cardiovascular outcomes in persons who have borne children. A thorough literature search was performed using search terms related to breastfeeding and cardiovascular events. Two independent reviewers were involved in the screening and selection of eligible studies.2
Moreover, the statistical analysis involved a primary analysis that compared the study-specific hazard ratios for maternal CVD events in breastfeeding and non-breastfeeding persons who have borne children, and a secondary analysis that clarified how hazard ratios for maternal CVD, CHD, stroke, and fatal CVD vary depending on the duration of breastfeeding.2

Results:
Following eligibility review, 11 articles discussing 8 distinct studies with data on 1,192,700 persons who have borne children were included in the systematic review and meta-analysis.2
Statistical data revealed that the study-specific hazard ratios for women who breastfed versus those who did not were 0.89 for CVD, 0.86 for CHD, 0.88 for stroke, and 0.83 for fatal CVD. Moreover, reported data showed that the relative risks for maternal CVD, CHD, stroke, and fatal CVD declined significantly with lifetime durations of breastfeeding up to 12 months.
Figure 1 shows the hazard ratios for breastfeeding across different lifetime durations; in the graph, a value below 1 suggests decreased risk.2
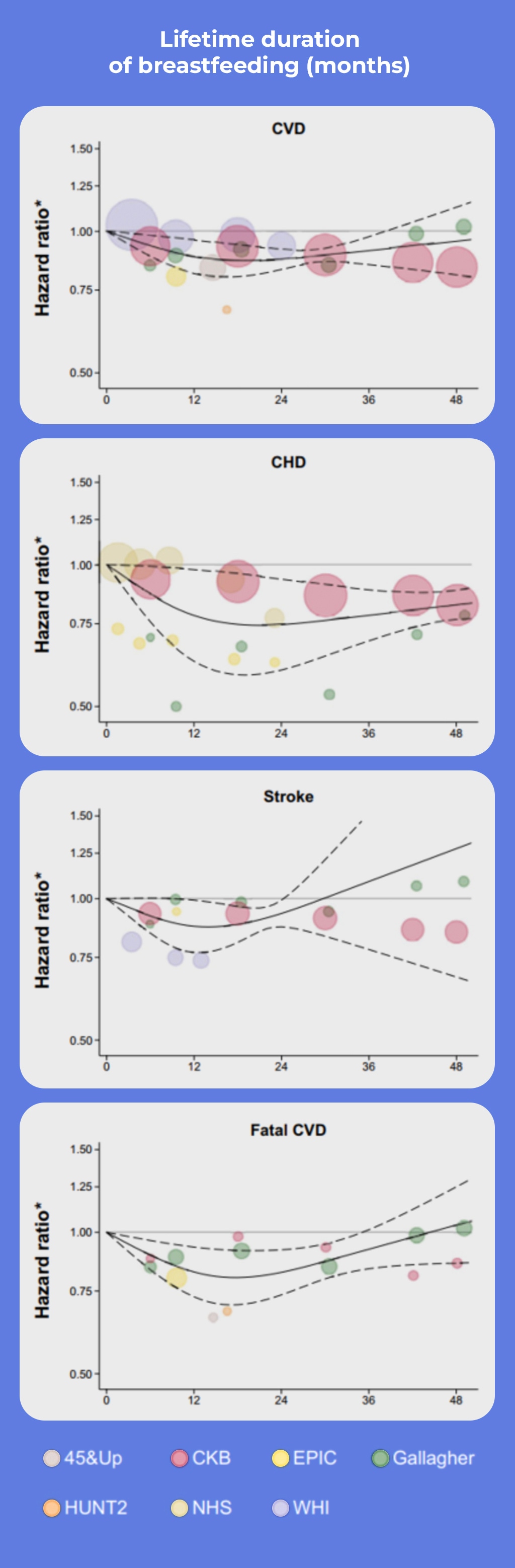
Figure 1. Hazard ratios for CVD events versus lifetime duration of breastfeeding.
Notes: *Comparing women with different lifetime durations of breastfeeding with parous women who never breastfed. 45&Up, 45 and Up Study; CKB, China Kadoorie Biobank; EPIC, European Prospective Investigation Into Cancer and Nutrition; HUNT2, Nord-Trondelag Health Survey 2; NHS, Nurses’ Health Study; WHI, Women’s Health Initiative.
Discussion:
Based on the combined study-specific hazard ratios, women who breastfed showed 11% lower relative risk for CVD, 14% for CHD, 12% for stroke, and 17% for fatal CVD events. Moreover, longer lifetime durations of breastfeeding for up to 12 months were associated with decreasing risk for maternal CVD, CHD, stroke, and fatal CVD events.2
Previous studies have provided possible explanations between the association between breastfeeding and reduced maternal cardiovascular risk. One possible explanation focuses on the role of oxytocin, which is essential for breastmilk ejection, in improving cardiovascular health. Oxytocin has been shown to reduce blood pressure, induce vasodilation and improve metabolic functions.3
Furthermore, the hypothesis that lactation resets maternal metabolism, particularly glucose and lipid homeostasis, after pregnancy may explain how breastfeeding contributes to reduced CVD risk. Lastly, increased lipid and glucose levels have been associated with increased CVD risk; thus, the resetting of maternal metabolism could help decrease the risk of heart disease.4
Conclusion:
The systematic review and meta-analysis provide evidence that breastfeeding is associated with significantly reduced maternal risk of CVD events, including CHD, stroke, and fatal CVD.2
References:
- Chowdhury R, Sinha B, Sankar MJ, Taneja S, at al. Breastfeeding and maternal health outcomes: A systematic review and meta-analysis. Acta Paediatrica. 2015; 104:96-113.
- Tschiderer L, Seekircher L, Kunutsor S, et al. breastfeeding is associated with a reduced maternal cardiovascular risk: Systematic review and meta-analysis involving data from 8 studies and 1192700 parous women. J Am Heart Assoc. 2022;11:e022746.
- Gutkowska J, Jankowski M. Oxytocin revisited: Its role in cardiovascular regulation. Journal of Neuroendocrinology. 2012; 24:599-608.
- Stuebe A, Rich-Edwards JW. The Reset Hypothesis: Lactation and Maternal Metabolism. Am J Perinatol. 2009; 26(1):81-88
If you liked this post you may also like


