The Pediatric Rome IV Criteria - What is New?
The Pedriatric Rome IV Criteria – What is new?
Ilan J.N. Koppen
FGIDs are defined by the Rome criteria, which were established by working groups of the Rome Foundation. These criteria are symptom based and based on literature and consensus meetings. The name “Rome” comes from the place where the first meetings took place.
The first Rome criteria were established between 1990-1994, but they were only for adults. In 1999 the first pediatric Rome criteria were published and these were basically a copy of the adult criteria. Then in 2006 much was changed: now the pediatric Rome criteria were based on pediatric research and a subdivision was made between neonates/ toddlers and children/adolescents because they show different kinds of FGIDs. The most recent publication was in 2016, where still the same sub- division was made (Chart 1).
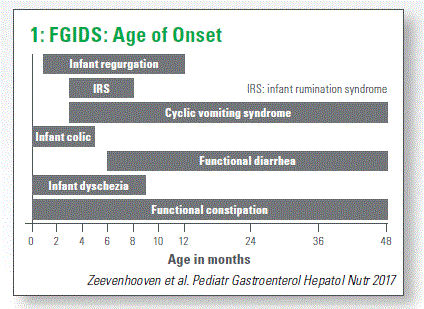
Reflux and Regurgitation
There are a lot of difficulties with the semantics of reflux and regurgitation because both clinicians and parents use the terms interchangeably.
![]() - Reflux (GER): passage of gastric contents into the esophagus
- Reflux (GER): passage of gastric contents into the esophagus
![]() - Regurgitation: reflux, which can be seen
- Regurgitation: reflux, which can be seen
- Reflux disease (GERD): reflux causing troublesome symptoms and/or complications
To define troublesome symptoms is a very difficult thing to do in young infants. The definition for infant regurgitation by Rome IV is that at least 2 events of regurgitation should occur per day for at least 3 wk in infants 3 wk – 12 mo of age and no retching, hematemesis, aspiration, apnea, FTT, feeding difficulties, abnormal posturing should occur and no other signs should be present.
The prevalence varies greatly from study to study and they say that between 8 – 26% of infants < 1 year of age have infant regurgitation and the peak is usually around 4 mo of age. Treatment consists of education reassurance, thickening of feedings and sometimes a positioning advice, although that is debatable.
GERD
There are rarer disorders like infant rumination syndrome, which is included in the Rome IV criteria. It is the habitual regurgitation of stomach contents into the mouth for the purpose of self-stimulation. In Rome IV it is defined as:
- Repetitive contractions of the abdominal muscles diaphragm, and tongue
- Effortless regurgitation of gastric contents, which are either expelled from the mouth or rechewed and reswallowed
- Three or more of the following:
* Onset between 3 and 8 mo.
* Does not respond to management for gastroesophageal reflux disease and regurgitation
* Unaccompanied by signs of distress
* Does not occur during sleep and when the infant is interacting with individuals in the environment (must include all for ³ 2 mo.)
According to prevalence studies, this would occur in 1.7–7.2% in infants < 1 year of age and in 1.9–2.9% in 1- to 3-year-old children, based on questionnaire and interview studies. However, this could be an overestimation.
Rumination is considered to be caused by social deprivation and parental behavior that does not meet the child‘s social needs, a child develops a behavior to self-stimulate. There is no diagnostic test required, but ask the parents to videotape. This is easy as now everybody has a mobile phone. Treatment consists of empathetic and responsive nurturing and parental training to deal with their child’s social needs in an appropriate matter.
Cyclic vomiting syndrome
For Cyclic vomiting syndrome Rome IV criteria stated:
- Two or more periods of unremitting paroxysmal vomiting with or without retching, lasting hours to days within a 6-mo period
- Episodes are stereotypical in each patient
- Episodes are separated by weeks to months with return to baseline health between episodes of vomiting
Prevalence: 0.0–3.8% in infants < 1 year of age, 3.4–6.1% in children 1–3 years. The etiology is not completely understood, but it is associated with a maternal history of migraine headaches.
Infant colic
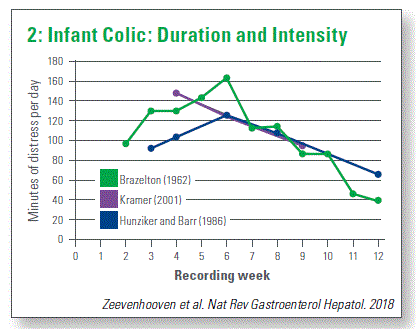
Infant colic consists of prolonged episodes of crying, often in the afternoon or evening, with peaks 4–6 wk of age, usually resolved by 3–4 mo of age. It can be very distressing for parents and is often a reason for consultation. But it has also been said to be part of neural developmental behavior and that it’s even part of normal physiology for child as well (Chart 2).
Rome III criteria were based on Wessel’s “rule of threes” (³ 3 hours/day, ³ 3 days/wk, ³ 3 wk). Du- ring the meeting for Rome IV, they asked: What is the evidence basis to use 3 hours as a limit? And is a child that cries for 2½ hours a less severe case? So they defined criteria for clinical purposes and for research purposes.
For the clinical diagnostic criteria, Rome IV states:
- 5 mo of age when symptoms start and stop.
- Caregivers report recurrent and prolonged periods of infant crying, fussing or irritability that occur without obvious cause and cannot be prevented or resolved by caregivers.
- No evidence of failure to thrive, fever or illness.
Additional for clinical research purposes:
4. In a telephone or face-to-face screening inter- view with a researcher or clinician, the caregiver reports that the infant has cried or fussed for > 3 hours per day during >3 days in 7 days
5. Total 24-hour crying plus fussing is confirmed to be > 3 hours measured by > 1prospectively kept 24-hour behavior diary
The prevalence for Infant colic is very high: 17–25% in infants £ 6 wk of age. The treatment consists of addressing parental coping in reassuring patients.
Functional diarrhea
A different kind of problem is functional diarrhea, which is considered as “frequent unformed stools in otherwise healthy toddlers” (“toddler’s diarrhea”). There are a lot of dietary factors to be considered, especially overfeeding, excessive fruit juice intake, other carbohydrates (fructose) ingestion with low fat intake, sorbitol.
Rome IV criteria:
- Daily painless, recurrent passage of ³ 4 large, unformed stools
- Symptoms last ³ 4 wk
- Onset between 6 and 60 mo of age
- No failure to thrive if caloric intake is adequate
The prevalence in infants is not very common; it is more commonly seen in 1- to 3-year-old children. Functional diarrhea usually resolves spontaneously before school age; the treatment consists of dietary evaluation and advice, education and reassurance.
Infant dyschezia
This is a very different problem, which is considered to be caused by failure to coordinate intra-abdominal pressure with relaxation of the pelvic floor.
Rome IV criteria:
- > 10 minutes of straining and crying before successful or unsuccessful passage of soft stools.
- No other health problems.
(This is in infants < 9 mo of age instead of < 6 mo in the Rome III criteria)
Prevalence is 0–3.2% in infants < 1 year of age. Treatment consists of education, reassurance and avoidance of rectal stimulation. There is no need for laxatives.
Functional constipation
Infrequent, difficult to pass, hard stools are suggestive of functional constipation. In toilet-trained children, fecal impaction can result in fecal incontinence. Its prevalence is very high, both in infants and toddlers (4.7–16.1% in infants < 1 year of age / 9.4–26.8% in 1- to 3-year-old children).
For Rome IV criteria at least 2 of the incidents must include 1 mo in children up to 4 years of age:
* 2 or fewer defecations per week
* History of excessive stool retention
* History of painful or hard bowel movements
* History of large-diameter stools
* Presence of a large fecal mass in the rectum neonates In toilet-trained children, the following additional criteria may be used:
* At least 1 episode/wk of incontinence after the acquisition of toileting skills
* History of large-diameter stools that may obstruct the toilet
Constipation in early infancy is often a reason to think of potential organic pathology (e.g. M. Hirschsprung, malformation). Later in life feeding changes are often related to the development of constipation and at a later age – when they‘re getting toilet trained – withholding behavior is a very big issue and big peak incidence of functional constipation is at 2–3 years.
First line of treatment for all children of all ages is polyethylene glycol. In children who have constipation and haven’t defecated for a while, disimpaction should be considered.
Conclusion
- FGIDs in infants/toddlers is diagnosed according to the Rome IV criteria
- Infant regurgitation and functional constipation are the most common FGIDs in infancy
- Functional constipation is the most common FGID in toddlers
- Not every FGID requires treatment (other than education and reassurance)